Guessing game ends
When we last left our hero, he was headed off to headline the Heart Ball. There we talked to Ari’s cardiologist and surgeon about whether we should have surgery on May 12 to replace his pulmonary valve.
Later that week we learned that while he looked good on the outside, an MRI showed his right ventricle was holding more than twice the blood it should, contributing to very high pressure. It was time to act before damage became permanent. We’ve been waiting a year and half to find out when we would do this. Now the guessing game was over.
Our last post-surgical hospital stay was 4 months. Doctors said if this surgery was smooth sailing—and there was no reason it shouldn’t be—he could be home as fast as 3-4 days. You’d figure they knew Ari by now…
Smooth sailing
Monday morning at pre-op, Ari had a grand old time running around the hospital. He likes to run as fast as he can (heart patient…not very fast), then dive face first on the floor. Exactly what we wanted before surgery: Ari mopping the hospital floor with his chest and face.
They took him around 7:30 a.m.
By 1 p.m., Ari was already up in CICU. His surgeon told us we did, indeed, achieve smooth sailing. All went well, the Mitroflow valve looked good, and now it was time for recovery.
Later that day they pulled his breathing tube. By 9 a.m. on Tuesday he was wide-awake and doing great! The plan was to pull his lines, chest tubes and the rest, and have him transferred to the recovery floor by night. Wednesday the plan was for him to be playing in the playroom.
Pulling chest tubes and lines can cause bleeding, so they decided to beef up Ari’s blood with a minor transfusion so he could clot better. It was done by 10 a.m.
By 10:30, Ari called the CICU into action stations, condition 1. He couldn’t breathe.
Action stations
The attending physician was leading 10 or so cardiologists, nurses, charge nurse, respiratory support, etc. like a general in the field. It was all “he’s de-satting” and “stat” and “get him captured” and so on. Ari had ‘em all out there steppin’ and fetchin’ like their heads were on fire and their asses was catchin’.
This went on for 2 hours until they ‘stabilized’ him on heavy cardiac meds and respiratory support. By the time the dust settled, Ari was critical.
This wasn’t supposed to happen.
Close your eyes and count your breaths for a minute. Go ahead.
The average adult takes 12 to 15 breaths a minute. After his acute respiratory crisis, when he was stabilized, Ari was taking as many as 110 breaths a minute. For a while, he was averaging 80 to 100 on BPAP.
Try putting a 2 year old in a tight, uncomfortable face mask. They don’t like it. They cry. When you cry, you don’t breathe well. If you need to keep a kid on BPAP so they can breathe, crying is a no-go. We had to hop him up on some pretty hefty medications: dexmedetodamine, morphine, medazolam, chloral hydrate, lorazepam to smooth him out. He was toast.
Soon we learned a new word: tachyphylactic. Being a former addict, Ari build up very fast resistance to these meds. While he was supposed to stay toasty, he would intermittently come out of it, get raging mad, and go completely off the rails. Not good for respiratory rehabilitation.
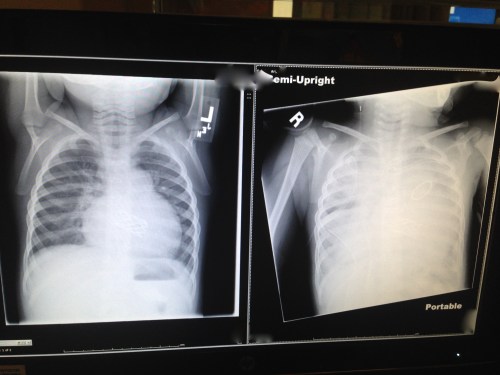
Worst of all, his lungs were so wet they looked snow white. On the left is his pre-op x-ray. The white shape in the middle is the outline of his (enlarged) heart. The black spaces between the ribs on the left and right indicate clear lungs.
On the right is his ‘snow white’ post-respiratory crisis x-ray. During the crisis, his lungs were so wet, he was foaming at the mouth.
Ari needed this fluid pulled out of his lungs, so a diuretics extravaganza began. As you might imagine, if fluid is being sucked out of every part of your body so you can pee it out, you’re gonna get thirsty. I’m sure he wanted to grab a gallon jug and go to town. But gallon jugs aren’t allowed. Or quarts, cups, ounces. Not even a milliliter.
For the next 84 hours or so, Ari was either heavily sedated, or rippin’ mad, screaming, “ WATER! WATER! WAAATTERRR!!! Ari want water.”
When he wasn’t screaming for water, he was begging for it. Crying for it. And we couldn’t do a thing but try quite unsuccessfully to soothe him. Much of the time he needed to be re-sedated.
Unquenchable thirst plus no food plus scary mask plus IVs all over him plus cracked chest plus sedation side effects = unhappy boy.
Funny thing about the water, though. Deep beneath his narcotic and sedation induced haze lurked our pretty smart kid. He kept asking for water and wasn’t getting anywhere, so he tried a few other angles. He asked for milk and then said, “Milk, then water,” with convincing look on his face. (This is what we say to him at home when he asks for water.) He didn’t get anywhere so he said to Erica, “Wash your hands and eat!” trying to inspire our home mealtime routine. After asking me for water a few times and getting the shaft, he changed the request. “Ari want…Pedialyte.” Trying to impress me with 50-cent words is a good idea, but unfortunately for Ari, we had to keep the bottles corked.
He just had to suffer. And suffering it was. 4 days. No break.
Set condition 2
Thursday night he started breathing a little easier. By Saturday morning, he had smoothed out enough to move to a nasal cannula and get the scary, painful mask off of his face.
Over the course of the day Saturday we started stepping down the sedation, which was a hefty mountain to climb down for such short time in the CICU. The attending physician took one look at his eyes and said, “Ari’s not organized right now.” So the goal was to try to find our boy hiding inside the raving lunatic.
This is where we are now, trying to get the sedation down and de-intensifying him. What’s most important is that he’s breathing easier and his chest x-ray is clearing. If it’s smooth sailing from here out…okay, I’m just gonna stop there.
P.S. Why did this happen? Was it Ari’s wonky heart not letting him recover from this surgery like a ‘normal’ cardiac toddler might? Some doctors believed so at first, but something wasn’t adding up. Several days ago, some doctors started thinking it was TRALI.
TRALI…transfusion related acute lung injury. It happens in about 1 in 5,000 blood transfusions. Just a random, rare, serious, and sometimes fatal complication.
It’s kind of like, “A funny thing happened on the way back from serious cardiac surgery. I aced the surgery, but then I got hit by a TRALI car.” 1 in 5,000…leave it to Ari.
P.P.S. Happy 2 year Rossaversary, Ari.
UPDATE: I was up with Ari all night. We turned off the heavy sedatives around 10 p.m. By 2 a.m., we were watching basketball videos and singing songs while sipping Pedialyte and milk. Neither of us has slept, and that’s just fine.
love you guys! Makes me cry thinking he has to suffer through thirst, what a smart guy trying any angle!! He is amazing. What sweet relief to finally see him be him and get to sip something!
XOXO
WOW! I am once again in awe of this strong resilient little guy! What a story! He had us all on the edge of our seats once again. And now we can all resume breathing. Mike, you and Erica are amazing. Thank you so much for this update which is so eloquently delivered with your fabulous wit and story telling. Fondly, kathie
xoxo…hugs and kisses Ari…thinking of you
Ari’s trials cause me to realize just how trivial some of my daily concerns really are. Is the grass getting too long? This side of the house really needs paint? How very minor!
“Fate is kind,
She brings to those who love,
The sweet fulfillment of their secret longing”
Ari is surrounded with so much love, he will do just fine.
http://www.rossfamilylove.blogspot.com/
I guess Gracie is one of the four you mentioned…she is a champion warrior if you care to read along. Her Melody valve was placed just before Christmas 2013 and she is doing great!!
Lord – brings to mind a saying my husband introduced me to: “If it weren’t for bad luck, he’d have no luck at all.” We know that Ari is an odds-beater, but this particular demonstration really wasn’t necessary – so just be the one-in-a-million kid that you are, “Danger”, and do that recuperation thing you do so well! Love to you all…
I am crying for you guys and thirsty thirsty Ari. I remember when Matthew was an infant after open heart surgery and you could tell how thirsty he was. The nurse let us cheat a little and have him suck a wet washcloth. (Love those CHB nurses so much!) I am thinking of you, praying for you, and sending love and good thoughts. Thank G-d that he is coming out of this crisis. Love wins.
Thank God, Thank Erica, Thank Mike, and Thank the hospital staff. I truly can’t imagine what those days and nights were like. Love to all and can’t wait to see our Ariman coasting on his bike.
I just love this boy!!!!!!! ‘Nuf said!!!!!
Bravo!
Thank you for the updates. Everything sounds much more positive!
Feeling so much gratitude! Sending love and prayers to Ari and family for continuing strength and recovery.
Wow, Ari likes to keeps things exciting doesn’t he? Praying that he keeps improving from here. Hope you feel better soon little guy!
love and prayers to the lil warrior Ari
You are never far from our thoughts and hearts. Hang in there, little man. You have shown such strength and courage, we are awed. Lots of hugs and kisses from the Lisauski.
Ari, you’re such a strong and brave little guy. My prayers will continue for as long as your heart desires *no pun intended*. You have many many people praying for your recovery but it is you who must go through the pains and suffering to strive to stay alive. You, along with the doctors and the help of heaven’s blessings are answering our prayers. A trooper, a soldier and a warrior in your own right, I thank you for your bravery, courage and answers to our prayers. You are an inspiration and a blessing to all who know you personally and virtually. Sending much love to you little Ari today and always ❤
I love you Ari and all my friends do as well. We are all praying for you to get strong and go home soon. Hang in there family.
I am preaching on a text that includes the reference to circumcised hearts this morning- so you and Ari have been in my thoughts all week- continuing to pray!
Thinking of all of you. Way to go Ari !!! Keep getting better. Hugs and kisses to all. Love you Ari
Just want you to know that my son with severe complex congenital heart disease turned 15 yesterday! Keep up the good work Ari – he is obviously a fighter! Hope this is the last bump in his recovery and praying he is home soon and running around!
Thoughts and prayers are with you, Ari, all the way. xo Hang in there Mike and Erica……
Continuing to pray for all of you!
What a roller coaster ride for poor Ari. Get well quickly, little man. The world is out there for you to explore.
Lots of love, hugs, kisses, prayers, and more good news, please!. I love you all. Auntie Sandi-Bubbie